CALEC surgery, an innovative procedure pioneered at Mass Eye and Ear, offers new hope for patients suffering from severe corneal damage. This groundbreaking technique, which involves the transplantation of cultivated autologous limbal epithelial cells, effectively utilizes stem cell therapy to regenerate the cornea’s surface. The clinical trial demonstrated promising results, with an impressive 90% success rate in restoring vision for participants with previously untreatable eye injuries. As ophthalmology treatments continue to evolve, CALEC surgery stands out, tapping into the potential of limbal epithelial cells harvested from healthy eyes. This advancement not only targets corneal repair but also represents a significant leap forward in eye injury treatment methodologies, bringing renewed hope to countless individuals facing vision loss.
Revolutionary in the field of ocular medicine, the CALEC method represents a transformative approach to addressing severe corneal injuries. By leveraging stem cell techniques to cultivate healthy limbal cells, this surgical intervention opens avenues for comprehensive corneal restoration in patients who have endured debilitating eye trauma. With advancements in ophthalmic therapies, the focus on regenerating critical components of the eye, like limbal epithelial cells, is reshaping treatment protocols and improving patient outcomes. As researchers delve deeper into corneal repair strategies, the implications of CALEC surgery hold promise for those grappling with the limitations of traditional eye injury treatments. This paradigm shift not only enhances the prospects for restoring sight but also signifies a new era in the application of stem cell therapy within ophthalmology.
Introduction to CALEC Surgery
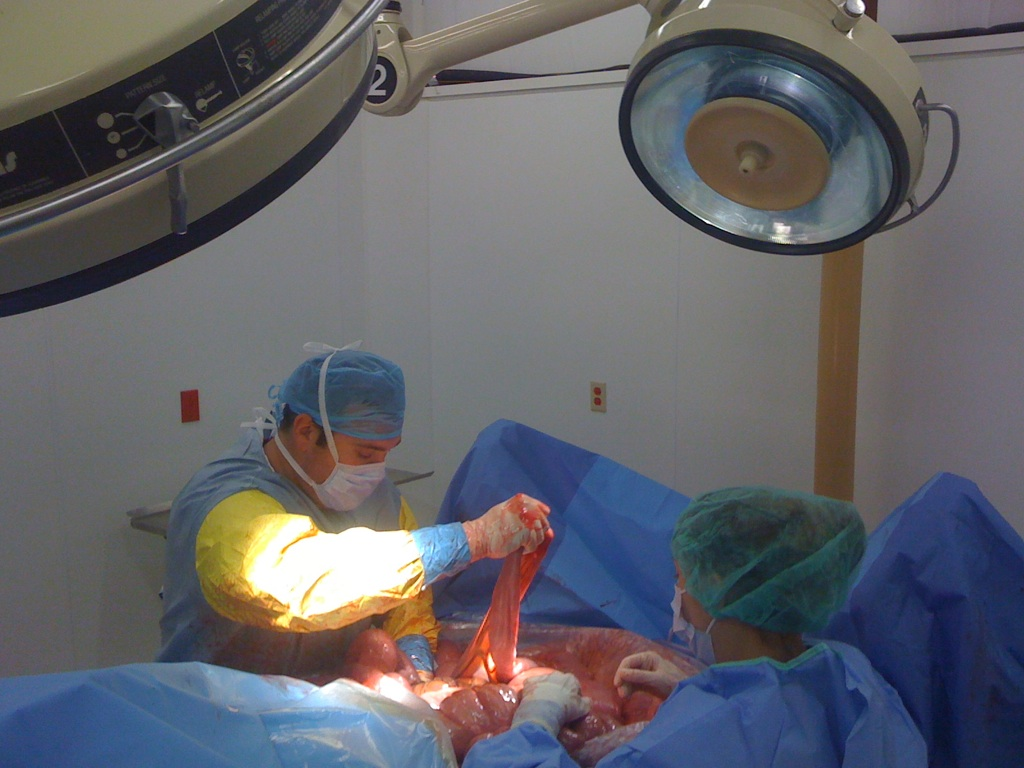
The recent breakthrough in ophthalmology treatments with CALEC surgery is a promising advancement for individuals suffering from severe corneal injuries. Cultivated Autologous Limbal Epithelial Cells (CALEC) surgery involves harvesting healthy stem cells from an unaffected eye, which are then cultured to create a graft that is transplanted into the damaged eye. This novel method allows for the restoration of the cornea’s surface, dramatically improving the quality of life for patients with previously untreatable conditions.
This innovative technique has showcased remarkable efficacy, with clinical trials demonstrating over 90 percent success in restoring corneal surfaces. Ula Jurkunas, the principal investigator at Mass Eye and Ear, emphasizes that this development not only signifies a leap in surgical procedures but also reflects hope for patients who have been living with persistent pain and visual impairments due to limbal stem cell deficiency.
Understanding Stem Cell Therapy in Corneal Repair
Stem cell therapy has transformed the landscape of ophthalmology treatments, providing revolutionary options for corneal repair. By utilizing limbal epithelial cells, which are crucial for maintaining the cornea’s integrity, the CALEC procedure represents a significant step forward. In patients with chemical burns, infections, or other traumas that severely damage the cornea, traditional interventions often fall short, leaving many with limited options.
The clinical trial of CALEC surgery has proven this regenerative approach to be both safe and effective. By restoring the cornea, patients can regain their vision and diminish recurring pain, which were previously thought to be enduring consequences of their injuries. This progress not only advances individual health outcomes but also enriches the field of eye injury treatment generally.
The Role of Limbal Epithelial Cells
Limbal epithelial cells are vital for the health of the cornea, acting as a barrier against toxins and pathogens while also aiding in the regeneration of the corneal surface. When these cells are lost due to injury, the cornea cannot heal properly, leading to complications that may result in vision loss. CALEC surgery addresses this vital need by utilizing stem cells sourced from the patient’s healthy eye, ensuring a biocompatible solution for their damaged cornea.
The focus on limbal epithelial cells highlights a crucial aspect of ocular health, as their depletion can lead to limbal stem cell deficiency. By employing stem cell therapy to cultivate healthy limbal cells, the CALEC method aims to restore not just vision but overall ocular functioning, offering a comprehensive solution for patients who previously faced bleak prognoses.
Mechanics of CALEC Surgery
The CALEC surgery process begins with the extraction of stem cells from the patient’s healthy eye through a minimally invasive biopsy. These cells are cultured over a few weeks, creating a viable graft that can be transplanted. This precision in manufacturing ensures that the graft meets strict quality control measures, essential for successful outcomes in transplant procedures. The entire process, from cell extraction to grafting, is designed to maximize patient safety and enhance recovery.
Clinical trials have shown that the transplantation of CALEC grafts results in a remarkable restoration of the corneal surface, showcasing a complete restoration rate of over 50% at three months. As patients progress through the follow-up phases, these success rates improve, further underscoring the effectiveness of the treatment for severely damaged corneas that were once deemed beyond repair.
Safety and Efficacy of CALEC in Clinical Trials
The safety profile of CALEC surgery has been a focal point in the clinical trials conducted at Mass Eye and Ear. With no serious adverse events reported in either donor or recipient eyes, and only minor complications occurring, the procedure demonstrates high tolerance among patients. The trial’s results, which show a substantive improvement in vision and corneal health, bolster the case for continued research and future application of CALEC surgery.
In addition to effective restorations, researchers noted that overall patient satisfaction increased significantly following the procedure. This dual focus on both efficacy and safety helps validate CALEC as a promising intervention in ophthalmology treatments, offering future potential for expansion into broader applications within eye injury treatment.
Expanding the Use of CALEC Surgery
As the CALEC surgery evolves, researchers envision expanding its applicability, particularly for patients with bilateral corneal damage. Plans for an allogeneic manufacturing process could pave the way for stem cells sourced from cadaver donor eyes to be used in transplant procedures, significantly widening the reach of this pioneering treatment. This anticipated development holds considerable promise for enhancing the quality of care for individuals facing dual eye conditions.
Implementing broader strategies will not only increase patient access but also foster advancements in research methodologies within stem cell therapy. Ongoing trials are anticipated to engage larger populations at multiple centers to refine techniques and ensure robust data supporting CALEC’s scalability and implementation in diverse patient demographics.
Research Collaborations Enhancing CALEC Development
Collaboration between research institutions has played a crucial role in the successful development of CALEC surgery. Partnerships between Mass Eye and Ear, Dana-Farber Cancer Institute, and Boston Children’s Hospital have facilitated the intricate process of both the research and manufacturing of stem cell grafts. This multidisciplinary approach ensures that innovative treatments are derived from evidence-based research while meeting regulatory standards for safety and efficacy.
Ongoing collaboration not only enriches the research surrounding CALEC surgery but also fosters an environment for shared insights that can lead to further innovations in ocular medicine. The involvement of various institutions also allows for a more comprehensive understanding of the impacts of stem cell therapy on vision restoration and overall ocular health.
Future Prospects of Stem Cell Therapy in Ophthalmology
The prospects for stem cell therapy within ophthalmology remain bright as advancements such as CALEC emerge from rigorous clinical trials. Investigations into the long-term effects of this innovative treatment will pave the way for validation and federal approval, potentially revolutionizing how we treat corneal damage. With the National Eye Institute’s backing, the future of CALEC and similar therapies appears promising.
Additionally, growing public and scientific interest in regenerative medicine is likely to accelerate the exploration and acceptance of such therapies. The potential to alleviate suffering and restore sight through patient-derived stem cell applications has far-reaching implications, not only for individuals affected by eye injuries but also for the broader landscape of ophthalmic care.
Conclusion: The Future of CALEC and Eye Care
As the landscape of eye care continues to transform through innovations like CALEC surgery, the future holds unprecedented potential for patients. By bridging the gap between laboratory research and clinical application, CALEC signifies a hopeful chapter in treating corneal damage with stem cell therapy. The commitment shown by researchers and institutions reflects a dedication to advancing ophthalmology treatments that can fundamentally change patient outcomes.
Looking ahead, expanding research into CALEC surgery could provide life-altering benefits for countless individuals. As further studies are conducted and the technology continues to refine, there is optimism that CALEC will become an accessible and routine option for patients facing serious corneal injuries, thereby enhancing their quality of life and vision.
Frequently Asked Questions
What is CALEC surgery and how does it work for corneal repair?
CALEC surgery, or cultivated autologous limbal epithelial cell surgery, is a groundbreaking procedure designed for repairing the cornea using stem cells. It involves harvesting limbal epithelial cells from a healthy eye, expanding them into a tissue graft, and transplanting this graft into a damaged eye. This innovative approach aims to restore the cornea’s surface, effectively treating injuries that previously had no viable treatment options.
How effective is CALEC surgery in treating corneal damage?
Research indicates that CALEC surgery is over 90 percent effective in restoring the cornea’s surface. Clinical trials have shown complete restoration of the cornea in about 50 percent of participants at the three-month follow-up, with success rates increasing to 93 percent and 92 percent at 12 and 18 months, respectively. This treatment holds significant promise for individuals with corneal injuries that were once deemed untreatable.
What are the benefits of using stem cell therapy in CALEC surgery?
The use of stem cell therapy in CALEC surgery allows for the regeneration of limbal epithelial cells that are essential for corneal health. By leveraging the patient’s own stem cells, CALEC minimizes the risks of rejection and provides a natural solution for corneal repair. This innovative technique is not only effective in surface restoration but also improves visual acuity for many patients.
What types of eye injuries can CALEC surgery help treat?
CALEC surgery aims to treat eye injuries that lead to limbal stem cell deficiency, such as chemical burns, infections, or trauma that damage the corneal surface. This procedure provides hope for patients suffering from vision impairment and chronic pain due to corneal injuries.
Are there any risks associated with CALEC surgery?
CALEC surgery demonstrates a high safety profile with minimal adverse effects reported in the clinical trials. The most notable was a mild bacterial infection in one participant, which was linked to chronic contact lens use rather than the surgery itself. No serious complications occurred, highlighting the procedure’s safety in treating eye injuries.
Is CALEC surgery currently available to patients?
Currently, CALEC surgery remains experimental and is not widely available at Mass Eye and Ear or any U.S. hospitals. Ongoing studies are needed to further validate the treatment’s efficacy and safety before it is submitted for federal approval.
What future developments are anticipated for CALEC surgery?
Future research aims to expand the use of CALEC surgery by developing an allogeneic manufacturing process using limbal stem cells from cadaveric donor eyes. This advancement could potentially enable treatment for patients with damage to both eyes, broadening the scope of effective ophthalmology treatments available to those with severe corneal injuries.
Who developed the CALEC surgery technique and what are its origins?
CALEC surgery was developed at Mass Eye and Ear by Ula Jurkunas and her team, building on nearly two decades of research into regenerating limbal epithelial cells. This innovative approach combines stem cell therapy with advanced surgical techniques to address corneal injuries that were previously considered untreatable.
| Key Points |
|---|
| First CALEC surgery performed at Mass Eye and Ear. |
| Transplanted stem cells successfully restored corneal surfaces in 14 patients. |
| Initial trial results showed CALEC is over 90% effective. |
| Procedure involves harvesting stem cells from a healthy eye. |
| The treatment addresses limbal stem cell deficiency. |
| Future studies hope to include patients with bilateral damage. |
| CALEC therapy is not yet available in U.S. hospitals. |
| Research is funded by the National Eye Institute. |
Summary
CALEC surgery represents a significant advancement in the treatment of corneal injuries that were previously deemed untreatable. The successful clinical trials at Mass Eye and Ear highlight the potential of cultivated autologous limbal epithelial cells to restore vision and improve the quality of life for affected patients. With ongoing research and further trials, CALEC surgery may soon become a viable treatment option for a broader range of eye injuries, paving the way for innovative solutions in ophthalmic care.